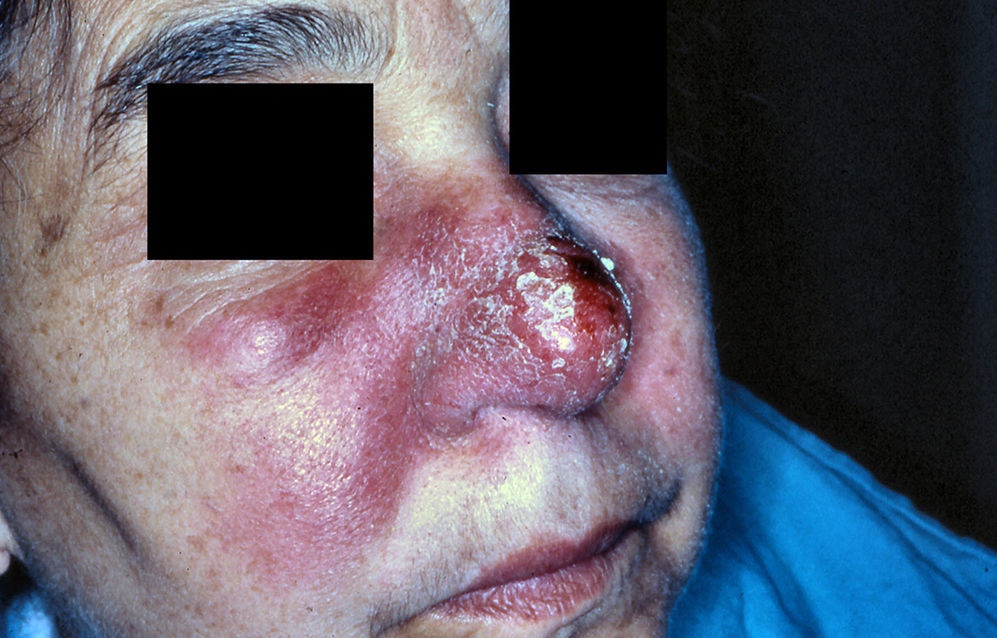
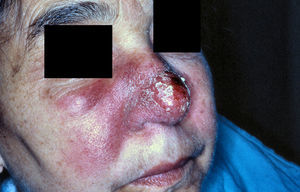
A 64-year old lady, known to have hypertension and urolithiasis, presented with a 4-month history of a slowly growing, erythematous-edematous and infiltrative plaque with superficial desquamation, involving all the nose skin surface – except for the root – and both zigomatic areas up to the naso-labial folds (Fig. 1).
The patient came from a remote rural area of the south-eastern Sicily, and was a farmer. Personal and familiar anamnesis was negative for autoimmune diseases or skin disorders.
Routine blood exams were within normal limits; serum autoantibodies (antinuclear, anti-ENA, anti-JO1 and anti-Scl70) were negative. Nailfold capillaroscopy and chest X-ray examination were normal.
Histopathologic examination of a cutaneous biopsy revealed a granulomatous infiltrate in the dermis, consisting of lymphocytes, histiocytes, and multinuclear giant cells with hyperkeratotic overlying epidermis. A touch-imprint preparation of a skin specimen, showed Leishmania amastigotes, within the histiocytes as well as extracellularly.
Lupoid leishmanniasis (LL) is a rare form of cutaneous leishmaniasis (CL) showing a striking resemblance with some other granulomatous skin diseases of inflammatory or infectious origin.1
In fact, LL is characterized by a typical spreading of the initial lesion leading to an infiltrated plaque with undefined borders, whereas some papules and nodules, often with scaling, may become apparent, presenting a lupoid aspect. The involvement of suggestive areas, as in our case, may further complicate the differential diagnosis.2
Histopathological features are that of epithelioid granulomas, and the detection of amastigotes is often hollow, both in microscopy and cultures.3
It seems that in LL certain strains replicate inside the macrophage, so assuming their ability to evade intracellular destruction or a concomitant defect in the T-cell activation process.2,3Leishmania infantum, the most frequent causative agent of CL in our geographic area, have been rarely linked with LL.1,4
The patient received N-methylglucamine-antimoniate, 1mL twice-a-week intralesionally (total of 7 doses), with progressive improvement.
Conflicts of interestThe authors declare no conflicts of interest.