A 57-year-old man presented with bilateral leg swelling, myalgia, weight gain, and reduced urine output for three months. He exhibited no signs and symptoms of urinary tract infection or sexually transmitted disease (STD). He reported a past medical history of diabetes mellitus and hypertension for 20 years, and bariatric surgery and abdominoplasty from about five years ago. Blood cell count was normal. Serum creatinine and creatinine clearance were 1.9mg/dL and 49mL/min, respectively. A 24-h urine collection revealed 19g of protein. These results were consistent with nephrotic syndrome. Serological tests for hepatitis and HIV were negative and the venereal disease research laboratory (VDRL) test was positive with a titer of 1:1024. The ultrasound showed normal kidney size with some suggestive features of acute parenchymal disease. He was treated with losartan, furosemide, hydrochlorothiazide, spironolactone, atorvastatin, heparin, and insulin, which resulted in a reduction of edema. Family members reported sudden personality changes and aggressiveness, pointing to a diagnostic of neurological syphilis disease. Computed tomography showed no abnormalities. VDRL and fluorescent treponemal antibody-absorption test were positive in cerebrospinal fluid, confirming neurosyphilis. A high-dose of intravenous crystalline penicillin was administered for two weeks. After 20 days, proteinuria was 17g and creatinine was 1.4mg/dL. A renal biopsy was performed. Light microscopy showed the glomeruli with a thick Bowman's capsule and interstitial fibrosis (Fig. 1A). The immunofluorescence was positive to IgG, C3 and lambda in glomerular basement membrane (Fig. 1B–D). Electron microscopy showed extensive diffuse foot process effacement, and subepithelial electron dense deposits (Fig. 1E and F). These results were diagnostic of membranous glomerulonephritis (MGN) secondary to syphilis. Three months after antibiotic treatment, renal function improved and a 24-h urine collection showed 1g of protein. Syphilis is a cause of MGN, which is not difficult to diagnose in a patient with a known history of this STD.1 However, syphilis may not be considered as the underlying cause of MGN in an undiagnosed patient,2 because of the rarity of this infection in a tertiary stage. If any feature is not compatible with idiopathic MGN or other common causes such as lupus, hepatitis B, nonsteroidal anti-inflammatory drugs, or malignancy, one should investigate uncommon causes of MGN as both treatment and outcome may change.
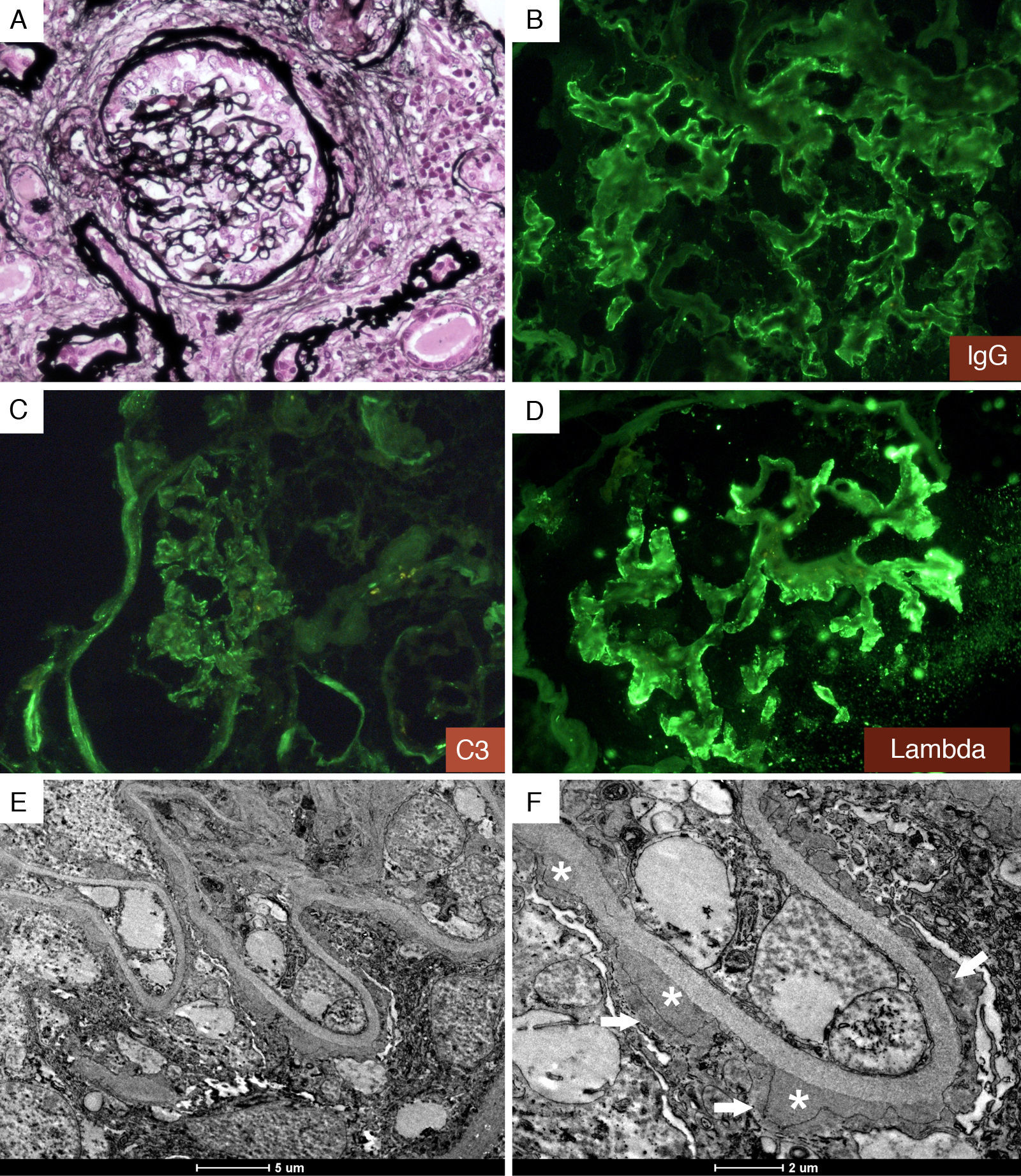
Membranous glomerulonephritis secondary to syphilis. (A) Glomerulus with a thick Bowman's capsule and interstitial fibrosis by Jones’ Methenamine Silver Stain. Immunofluorescence showing positive staining in glomerular basal membrane for IgG (B), C3 (C) and lambda (D); (E) and (F). Transmission electron microscopy showing extensive diffuse foot process (arrow) and subepithelial electron dense deposits (asterisk).
The authors declare no conflicts of interest.