Infections remain the most frequent cause of fever of unknown origin (FUO) in developing countries. Some cases of fever remain a mystery and patients are discharged without knowing the cause. Prehospital healthcare facilities vary between countries, and even within the same country. FUO was first described in 1961 by Petersdorf and Beeson when they established the three criteria that define FUO: a minimum measured temperature of 38.3°C, febrile states occurring on several occasions over a period of at least three weeks, and a minimum of one week of investigations being required.1 The modern definition of FUO is based on modifications of these criteria taking into account four specific patient subtypes: classic, nosocomial, immunedeficient (neutropenic), and HIV-associated FUO.2,3
We outlined changes in causes of classic FUO according to the latest definition and compare the causes with those of a previous study conducted at the same hospital in 1974.4 We retrospectively reviewed 374 adult patients with FUO admitted to the Abbassia Fever Hospital under the definition outlined by Durack and Street (1991).5 Data were obtained from admission files. The patient population comprised 217 (58%) male patients, with a mean age of 40.2±14.5 years. Further, 240 patients (64.2%) lived in urban areas, while 134 (35.8%) lived in rural areas.
A continuous pattern of fever was found in 211 patients (58.3%), while 58 patients (16%) presented with a remittent pattern, and 87 patients (23.2%) showed intermittent fever symptoms. Six patients (1.6%) had relapsing fever.
Blood cultures grew Gram-negative organisms in only nine cases (2.4%) and Gram-positive in eight cases (2.1%). Also, in urine cultures Gram-negative organisms were dominant including E. coli, Klebsiella and Enterobacter while Gram-positive cocci were only S. aureus.
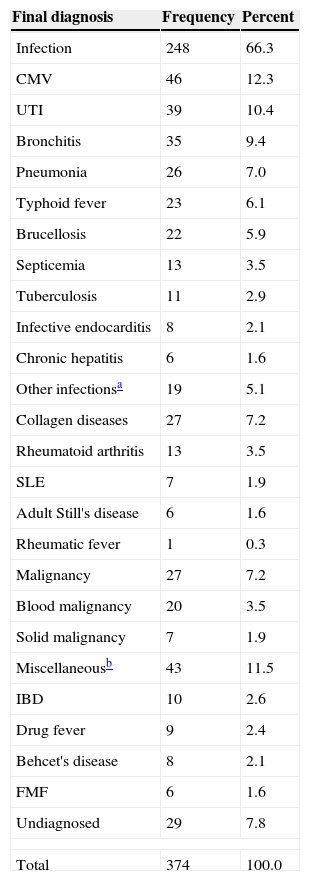
With regard to the final diagnosis, 248 patients (66.3%) were diagnosed with an infection etiology for FUO. Of these patients, 46 had cytomegalovirus infection (CMV). Among the non-infection patients, 49 (13.1%) were categorized in the miscellaneous group, and 29 (7.8%) were discharged without a final diagnosis (Table 1)
Final diagnosis in the studied population.
| Final diagnosis | Frequency | Percent |
|---|---|---|
| Infection | 248 | 66.3 |
| CMV | 46 | 12.3 |
| UTI | 39 | 10.4 |
| Bronchitis | 35 | 9.4 |
| Pneumonia | 26 | 7.0 |
| Typhoid fever | 23 | 6.1 |
| Brucellosis | 22 | 5.9 |
| Septicemia | 13 | 3.5 |
| Tuberculosis | 11 | 2.9 |
| Infective endocarditis | 8 | 2.1 |
| Chronic hepatitis | 6 | 1.6 |
| Other infectionsa | 19 | 5.1 |
| Collagen diseases | 27 | 7.2 |
| Rheumatoid arthritis | 13 | 3.5 |
| SLE | 7 | 1.9 |
| Adult Still's disease | 6 | 1.6 |
| Rheumatic fever | 1 | 0.3 |
| Malignancy | 27 | 7.2 |
| Blood malignancy | 20 | 3.5 |
| Solid malignancy | 7 | 1.9 |
| Miscellaneousb | 43 | 11.5 |
| IBD | 10 | 2.6 |
| Drug fever | 9 | 2.4 |
| Behcet's disease | 8 | 2.1 |
| FMF | 6 | 1.6 |
| Undiagnosed | 29 | 7.8 |
| Total | 374 | 100.0 |
Comparing the findings of the present study with a similar study conducted in 1974 that examined 129 patients with FUO in the same hospital,4 we found that infections still represent the main cause of FUO in Egypt (66.3% vs. 60% in 1974); however, the percentage of undiagnosed cases has dropped from 12% to 7.8%. Salmonella infection was diagnosed in 23 of 248 cases of infection, while brucellosis accounted for 22 cases.
Infections remain the predominant cause of FUO in Egypt; however, the causative agents have changed over the last 40 years. The proportion of undiagnosed cases of FUO seems to be lower than what it was in the past due to advances in diagnostic technologies. Finally, clinicians must be aware that the etiology of FUO varies across demographics, geography, and time. Accordingly, reporting local cases is important in informing clinicians about the epidemiologic pattern.
AuthorshipProf Mohamed Fawzy Montasser: Chosen the research idea and revised the results Ass. Prof Nadia Abdelaaty: follow up data collection, revise the results and wrote the manuscript. Dr Iman Montasser: data analysis, wrote and submitted the manuscript, Dr Ahmed El Khouly: Data collection, statistical analysis.
Ethics statementThis study was carried out after approval of Research and Ethics Committee of Ain Shams University, Cairo, Egypt in accordance with local research governance requirements. All human studies have been approved by the appropriate ethics committee and have therefore been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and all subsequent revisions.
Sources of fundingThis research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
Conflicts of interestThere are no financial or other relations that could lead to a conflict of interest.