Advances in the treatment of HIV infection in the last decades have increased life expectancy of these patients and raise the question of what kind of effect chronic infection and its treatment might exert on the behavior of age-related conditions such as neurodegenerative diseases.
Patient dataWe performed a retrospective analysis of patients’ records to assess the frequency of the association between HIV infection and parkinsonian symptoms in our hospital population. Among 249 records we identified four individuals with reported parkinsonian symptoms initiated after HIV diagnosis. Three of them had no other identifiable cause of secondary parkinsonism. All had symptom onset before the age of 60. Based on this study sample one could estimate an incidence rate of nearly 101 per 100.000 person/year, which is similar to the risk of Parkinson's disease in the general population above 70 years.
DiscussionThese findings suggest that HIV infected individuals might be at a higher risk for developing parkinsonism as a manifestation of early neurodegeneration. Prospective and larger studies are needed to address this particular association and its characteristics.
Manifestations of neurodegenerative conditions have become increasingly important in the evaluation of HIV-infected (HIV+) patients with chronic infection and adequate response to antiretroviral therapy (ART). This could be justified by the increasing life expectancy of this population, but studies also indicate that these individuals are at higher risk of developing symptoms of neurologic conditions earlier than the general population even in the absence of immunosuppression or opportunistic infections.1 Research on this area has tried to define if chronic asymptomatic HIV infection could be the direct cause of these symptoms or some kind of induction agent capable of triggering an early presentation of neurodegenerative diseases that would develop regardless at older age, and whether treatment choices for HIV influence the occurrence of these conditions as protective or harmful agents. Based on the findings of Tisch and Brew2 we are involved in a study to assess the frequency of the association between HIV infection and parkinsonism in our population. This is a retrospective review of patient records from our Infectious Disease and Neurology clinics. Herein we present data from HIV+ patients currently followed, among which we identified cases of parkinsonism initiated after the diagnosis of HIV.
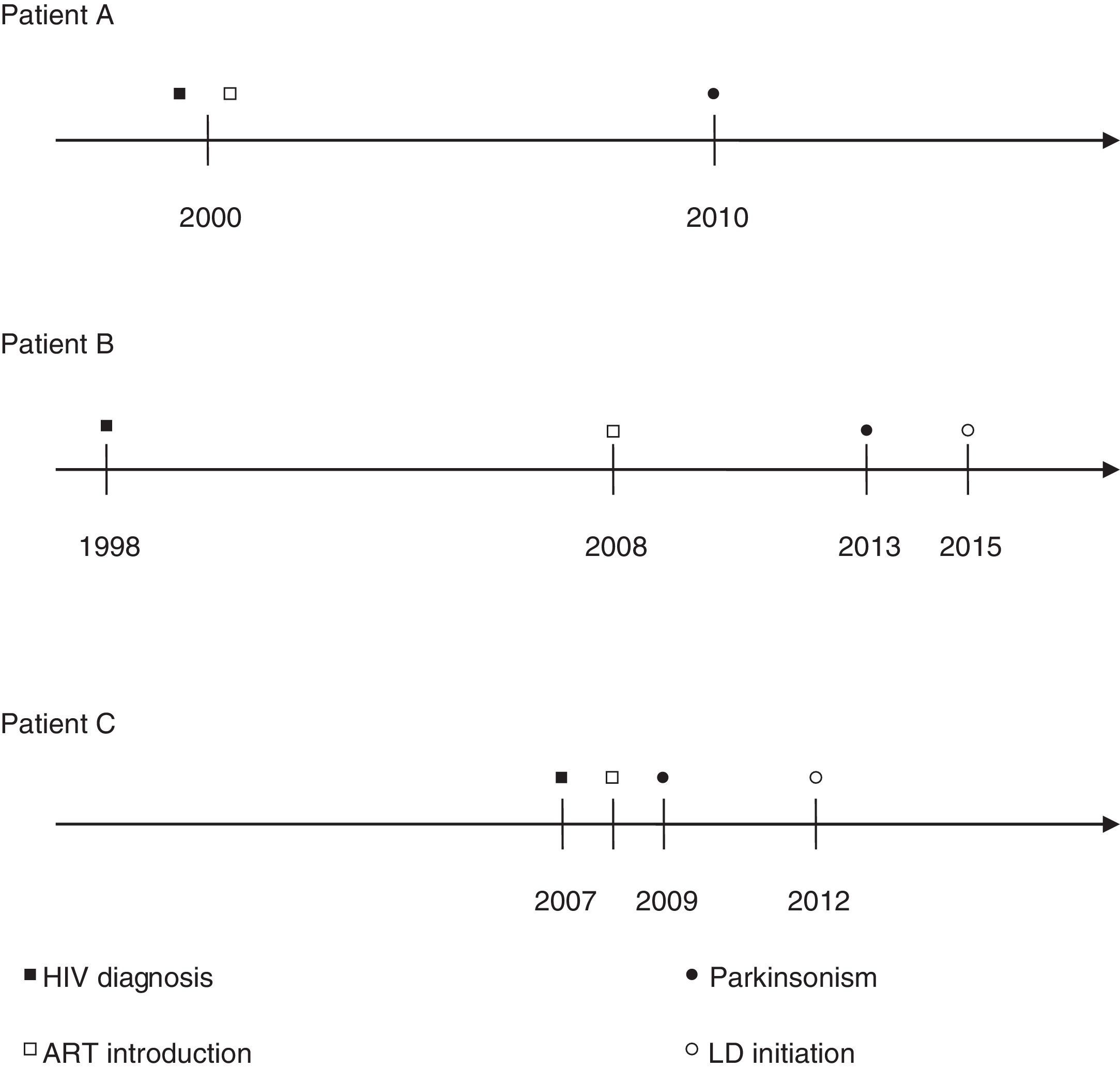
Patient dataThe study design has been approved by the Pedro Ernesto University Hospital Ethics Committee. We retrospectively analyzed, from April to October 2015, a total of 249 records from patients diagnosed with HIV, of which 36.6% were females and 63.4% males, with a mean age of 47 years and a mean length of disease of 12 years (0–33 years). Four individuals were diagnosed with parkinsonism, but one of them had neurotoxoplasmosis lesions that could explain the symptoms. The other three cases were men who had at the time of the parkinsonism presentation ages between 46 and 55 years and good adherence to ART with reported plasma viral loads below 50copies/mL and CD4+ cell count above 350permm3. None of them had a history of exposure to substances that could induce secondary parkinsonism, (neuroleptics, calcium channel blockers, or antiemetics). Neuroimaging disclosed a retrocerebellar cyst in patient C, and was unremarkable on the other two. At the beginning of parkinsonian symptoms, all patients were on the same ART as in the last follow-up visit. Patient A was under ART with tenofovir (TDF), lamivudine (3TC), atazanavir (ATV) and ritonavir (r), had no cognitive complaints and a last reported Mini Mental State Exam (MMSE) of 29/30; he had mild bilateral bradykinesia in upper extremities and postural, rest and kinetic tremor in the right arm that did not interfere with activities of daily living and therefore was not on any antiparkinsonian drug. Patient B was on zidovudine (AZT), 3TC and efavirenz (EFV), had no cognitive complaints and a MMSE of 30/30; he presented mild rigidity and bradykinesia in the right side, moderate neck rigidity, reduced arm swing, anteflexion of the trunk and postural instability. Patient C was also under treatment with AZT, 3TC and EFV, had no cognitive complaints and a MMSE of 27/30; he had mild symmetric bilateral rigidity and bradykinesia, mild rest tremor in the right arm, mild bilateral postural tremor in upper extremities and reduced arm swing. Patients B and C had a good response to levodopa (LD) even at low dosages (both with 200mg/day) and no significant side effects. Fig. 1 displays individual timelines highlighting the most relevant events from HIV diagnosis until last recorded follow-up.
Timelines showing evolution to parkinsonism after HIV diagnosis, highlighting initiation of ART and LD treatments. The timelines show the evolution to clinical manifestations of parkinsonism in each patient after the diagnosis of HIV and start of ART, LD initiation is also highlighted. All of them had at the beginning of the symptoms adequate viral control (<50copies/mL) and CD4+ cell count above 350permm3.
The incidence of neurodegenerative conditions, such as Parkinson's disease (PD), increases with age and HIV chronic infection seems to have a potential harmful effect increasing their risk even in younger individuals. The mechanisms whereby HIV favors the occurrence of degenerative changes in the central nervous system (CNS) were suggested in several experimental models. Disruption of the blood-brain barrier function as a fundamental mechanism facilitating the entrance of HIV in the CNS followed by a conjunction of direct and indirect viral factors, such as viral proteins gp120, tat and vpR has been observed. Also, cytokines and chemokines produced by macrophages/microglia and activated astrocytes (TNF-α, IL-6, GM-CSF, IL-1β) which induce neuronal damage mediated by oxidative stress, excitotoxicity and distress of cellular defense mechanisms (heat-shock proteins – HSP, chaperones and ubiquitin-proteasome system) with consequent apoptosis.3–5 Some antiretrovirals are also studied as potential agents of cellular damage, particularly protease inhibitors through inhibition of P-glycoprotein system,3 and “high” CNS penetration potential of combined ART might play a neurotoxic role6 although this is yet to be determinate. Khanlou et al. used immunohistochemical assays in cerebral tissue derived from autopsies of 73 HIV+ individuals aged 50 years or older. A higher expression of α-synuclein in the substantia nigra compared with control samples (16% vs 0%) even in asymptomatic patients was found, suggesting a relation between these neurotoxic mechanisms and the physiopathology of PD and other neurodegenerative diseases.7
In our study we have found three cases of HIV+ patients under effective ART who began PD symptoms prior to 60 years of age, with an estimated incidence rate of nearly 101 cases per 100,000 person/year which is similar to the incidence in those above 70 years in the general population.8 However studies with larger sample sizes are needed to make statistical relevant considerations. Other important limitations of our study were the incomplete or absent information (i.e. exposure to environmental toxins, family history) due to the retrospective nature of the study, unavailability of functional neuroimaging (DAT-SCAN, SPECT), and the lack of previous cerebrospinal fluid (CSF) analyses from the three reported patients.
We believe that the cases herein described are illustrative of parkinsonism as an early manifestation of neurodegeneration induced/facilitated by chronic asymptomatic HIV infection despite adequate ART. This report adds up to the few patients already described in the literature in an attempt to better characterize causal relation and clinical features of this condition. Clinically the reported cases of parkinsonism initiated after the prescription of adequate ART in HIV+ individuals including the ones described here, present similar signs and symptoms of idiopathic PD, with variable response to LD.2,9 To our concern there are no prospective studies to date evaluating long term prognostic aspects of these patients.
Difficulties to draw definitive conclusions from clinical research focused in the identification of neurodegenerative disorders and their association with HIV is hindered by variations of gender, age, and comorbidities compared with the general population, along with selection and survival biases in the studied samples.10 Prospective multicenter studies enrolling a larger number of patients are necessary to address the uncertainties related to causal factors, clinical characteristics, and prognostic aspects of these conditions.
Conflicts of interestThe authors declare no conflicts of interest.