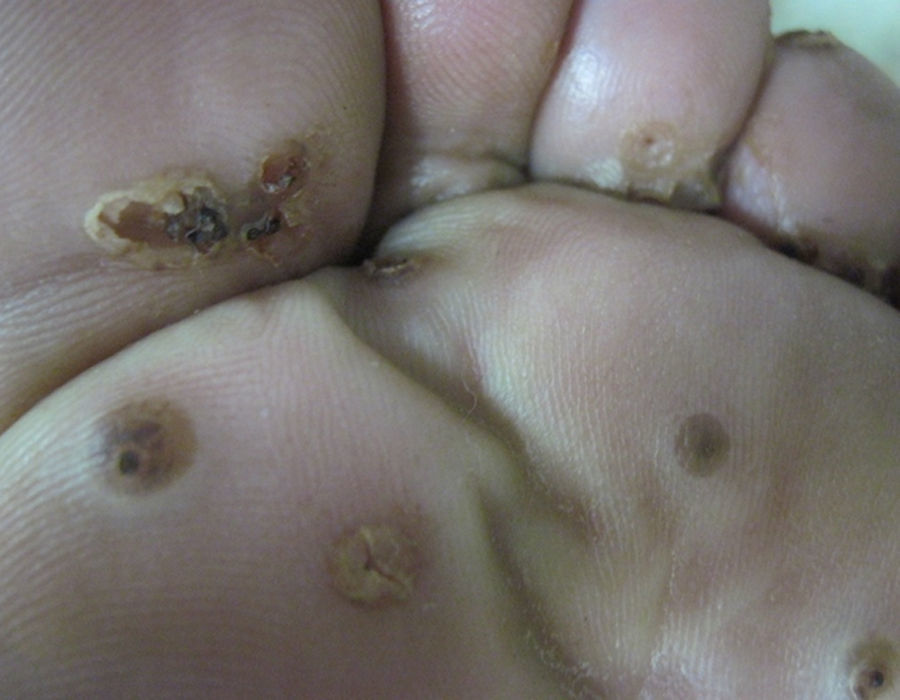
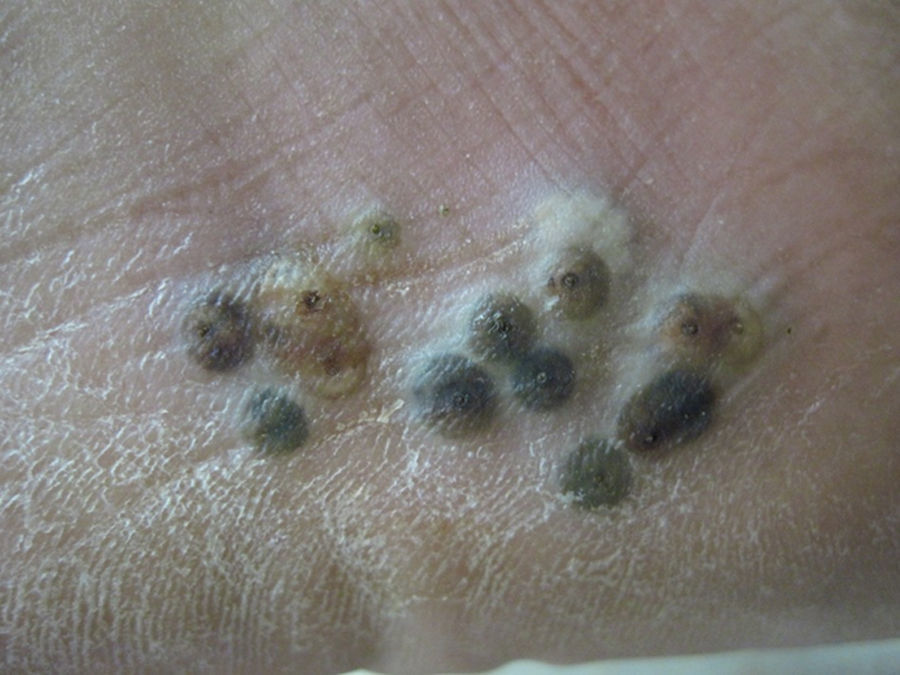
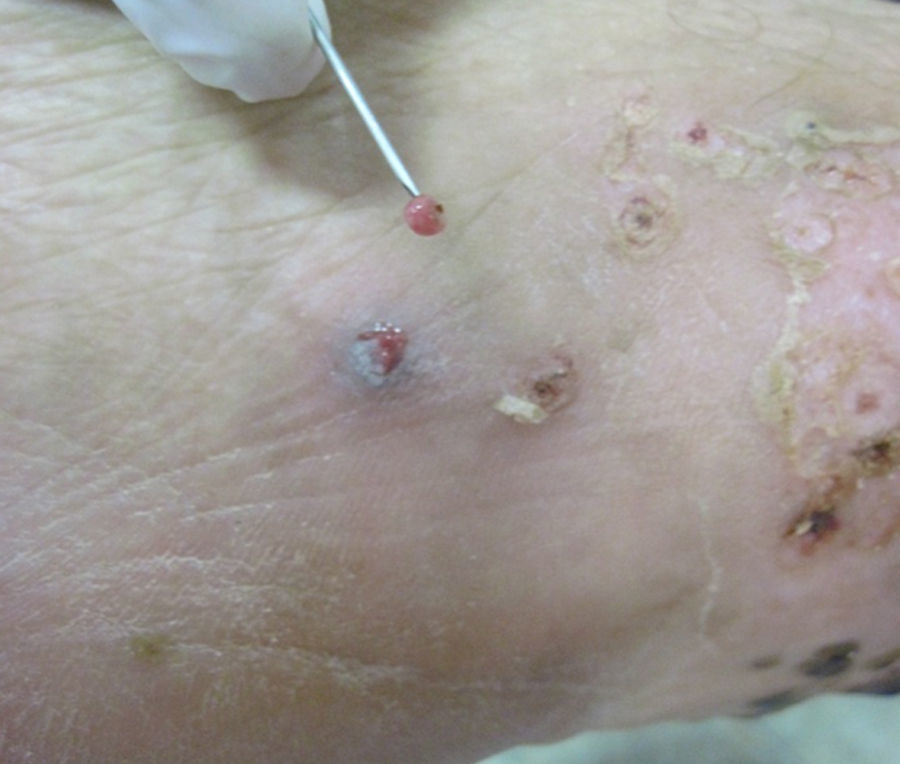
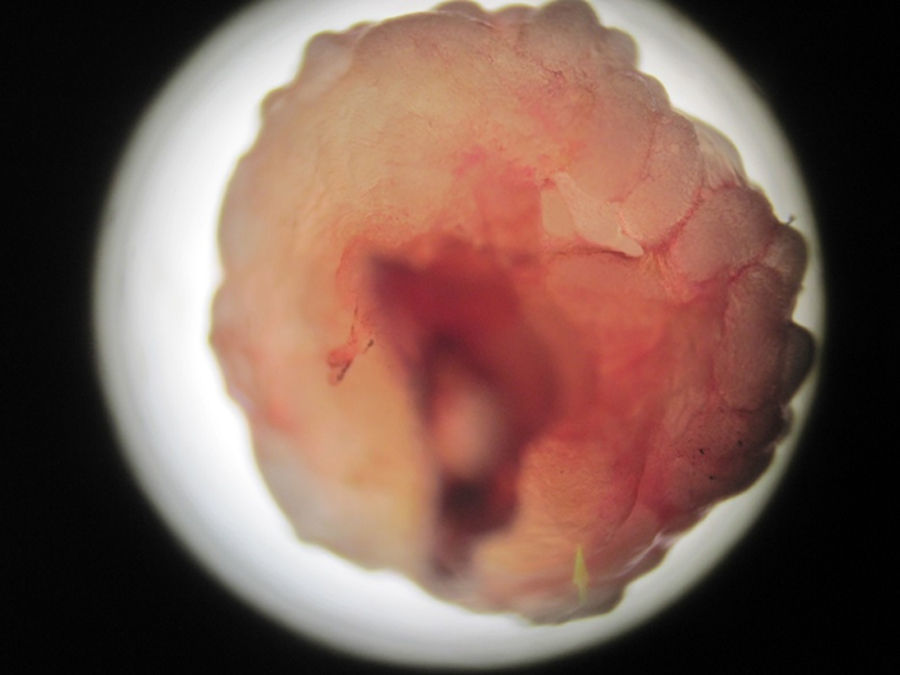
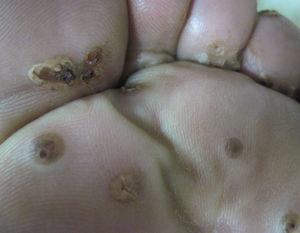
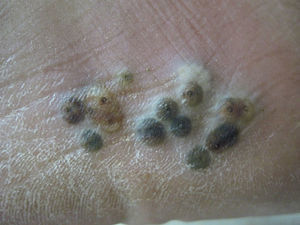
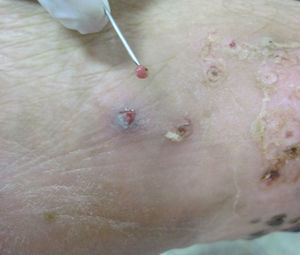
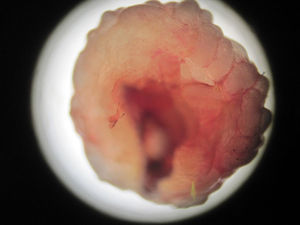
A 60-year-old male pig-farm worker from a rural area of Colombia was referred to our clinic with history of itchy skin lesions on the soles in the last two months. The patient reported often walking barefoot. Physical exam revealed clusters of monomorphic yellowish-brown papules and nodules with central black dots and indurated halos on the soles (Figs. 1 and 2). Treatment consisted of surgical extraction of embedded fleas from the lesions (Fig. 3) and adjuvant keratolytics. A flea (Tunga spp.) and its eggs were visualized with light microscopy in one of the excised lesions (Fig. 4). At clinical follow-up, the patient had recovered completely.
Tungiasis is an ectoparasitic skin disease caused by the penetration of the pregnant female sand flea Tunga spp. into the epidermis.1,2 This neglected tropical disease is an important healthcare issue due to its significant morbidity and endemicity in several Latin American countries, the Caribbean, and sub-Saharan Africa, particularly in resource-poor communities.3 However, several cases have been reported throughout the world in travelers returning from endemic areas. Although any location of the skin can be affected, lesions predominantly occur on the feet after contact with sand or sandy soil containing fleas. In some instances, tungiasis is associated with physical disability, chronic pain, skin complications and secondary bacterial superinfections.1,2 Diagnosis is clinical and may be challenging even to physicians in endemic areas as the clinical presentation varies with the developmental stages of the flea. An effective treatment involves excision of the fleas. Both people living in endemic places and travelers visiting these places should be advised to permanently wear closed shoes and socks. It has been shown that prevention of re-infestation leads to a reduction of the morbidity associated with tungiasis.4
Author contributionsClaudia J. Díaz contributed to conception of the manuscript and data acquisition.
Kevin Escandón-Vargas drafted the manuscript and made the literature review.
Both authors gave final approval of the version to be published.
Conflicts of interestThe authors declare no conflicts of interest.